Food poisoning: When food goes wrong
Salmonella poisoning has almost doubled in the past decade. Following a spate of local and international incidents, we investigate why this is happening.

Ash Lewis was limp in his mother's arms. The three-year-old boy had been sick for several days, in and out of the family doctor's surgery and up all night with diarrhoea. That Sunday he had been happily playing on the beach at Torquay on Victoria's west coast and later munching on an egg and cheese roll at a beachside cafe. He and his mother had left Melbourne to escape February's heatwave.
By Thursday his condition had gone downhill fast. He stopped speaking and couldn't walk. His parents, Scott and Sarina Lewis, rushed him to the Royal Children's Hospital in Melbourne. His blood pressure was down, his heart rate was low and his face was the ''colour of concrete''. From the happy little boy playing in the sea he was now in hospital with an IV drip in his arm.
An estimate by the federal Department of Health puts the number of Australians contracting food-borne illness at 5.4 million cases, or nearly one in four, with 120 people so seriously affected they die. The cost to the economy has been put at $1.25 billion.
While outbreaks of the deadly bacterial toxin botulism and food-borne hepatitis A are on the decline, incidents involving salmonella have almost doubled in the past 10 years, from 6990 in 2003 to 12,836 in 2013. In Brisbane last year, 220 people became ill and one elderly woman died after a Melbourne Cup lunch. The finger was pointed at raw egg mayonnaise contaminated with salmonella. In 2010, salmonella-contaminated aioli made with raw egg was found to be the cause of an outbreak in a hamburger bar that struck down 179 people.
Since Ash became ill, the numbers for the Torquay outbreak have ratcheted up, with a further 63 people confirmed to have been affected by an outbreak of food poisoning linked to the Bottle of Milk cafe. The Victorian Department of Health believe another 123 people may have been affected. A stool sample taken from Ash confirmed he was infected with salmonella bacteria causing gastroenteritis. The sandwich he ate at that cafe was prepared with mayonnaise made with free-range eggs. Owners of the cafe we spoke to believe this is the most likely cause of the food poisoning.

Food poisoning
WHAT IS IT?
Most food poisoning cases in Australia are caused by bacteria. Number one culprit is campylobacter with 14,672 confirmed cases last year, down from 10 years ago. The bacteria is found in raw meat and poultry, carried by pets and flies. The bugs build up in the gut and can cause gastroenteritis within two to five days. Campylobacter bugs are killed during cooking.
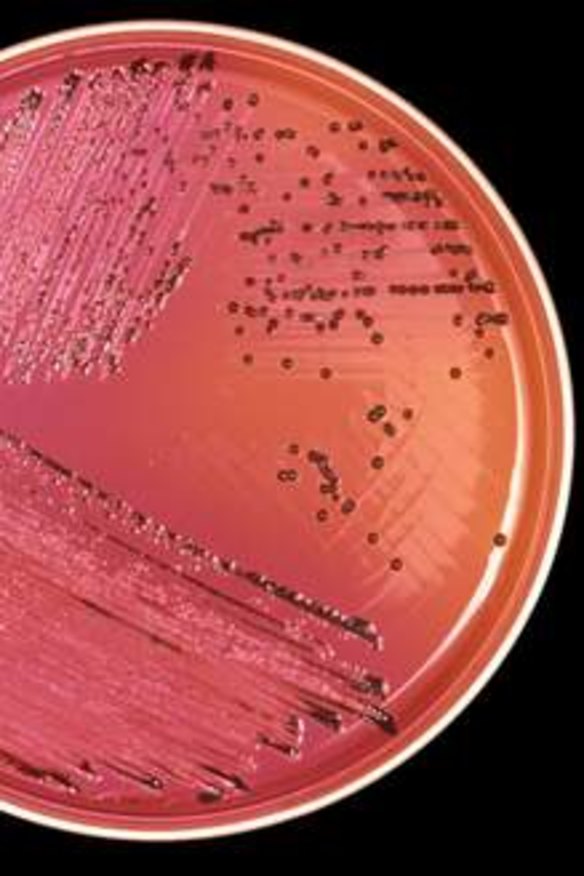
Salmonella strikes faster, within six hours, but can incubate in the gut for three days before nausea, cramps, diarrhoea, fever and headache set in. Foods that present the highest risk of salmonella contamination are undercooked chicken and food made with raw eggs such as mayonnaise.
Another nasty bug that causes food poisoning is Staphylococcus aureus, or golden staph, which struck 22 people in Sydney who ate chicken stir-fry at an elite sporting event in 2012. Six were admitted to hospital.
S. aureus is a bacteria that lives on our skin, gets into food from uncovered wounds, and, if it gets into food before being cooked, can grow and multiply. Unlike salmonella, which is usually killed during cooking, S. aureus produces a toxin that isn't destroyed in normal cooking. The toxin kicks in within one to eight hours, causing acute nausea and vomiting.

There is another bacteria that lives in the soil. It is found in rice and produces spores that can also survive cooking. Called Bacillus cereus, it causes problems when cooked rice is kept in the food danger zone - temperatures between 5 degrees and 65 degrees.
While we live comfortably with E. coli in our gut, some strains produce toxins that can cause dysentery while others can cause a blood disorder and kidney failure. Food poisoning from E.coli is rare in Australia but on the increase worldwide.
Food poisoning particular to fish include ciguatera. Victims become ill from toxins that have accumulated in large reef fish that have consumed smaller fish that in turn have feasted on toxin-producing plankton. An Australian mother and daughter died in Bali earlier this year from scromboid, caused by histamine that develops as amino acids break down in fish that have not been handled safely.

WHAT CAUSES IT?
"The biggest cause of food poisoning is lack of knowledge and a lack of awareness," says Juliana Madden, executive officer of the Food Safety Information Council. Food safety "is not about being paranoid but using common sense".
She pinpoints three areas in the kitchen where things can go drastically wrong. "Poor hygiene has to be avoided at all costs."

Madden says if cooks washed their hands after using the toilet and blowing their nose, cases of food poisoning would be greatly reduced.
"We have a culture where we assume we are clean, but how many men wash their hands after using a public toilet? Hygiene comes from personal attitude."
Cross-contamination - bacteria transferred from one food to another - is another critical point in food preparation. For example, if raw chicken (a source of salmonella) is placed on a chopping board on which the ingredients for a potato salad are subsequently prepared, the bacteria can multiply in the salad.
Salmonella can occur naturally on poultry and can be passed on to eggs at the time they are laid. Food Standards Australia New Zealand states: "The frequency of salmonella-contaminated eggs in Australia is very low. Despite this, there is a potential risk of illness from consumption of raw or lightly cooked eggs, or the consumption of uncooked foods containing raw egg.''
The other crucial factor for the development of food-borne diseases is the combination of time and temperature. "Most dangerous bugs love the temperatures we like," says Madden. "Food that is not being served straight away needs to be kept below 5 degrees or above 65 degrees."
Bacteria reproduce exponentially, so the longer at-risk ingredients stay in the ''danger zone'', the greater the risk. Madden says steak tartare - raw chopped beef with raw egg yolk - is ''risky, like eating puffer fish". "It is absolutely delicious but needs to be prepared by experts proficient in safe food handling."
During recent heatwaves across the nation, temperatures in restaurant kitchens have soared to around 50 degrees, says the president of Restaurant and Catering Australia, Matteo Pignatelli. "This has seen chefs having to change the way they cook," he says. "On days of extreme heat, chefs have to cook food straight from the fridge, whereas at other times they can have food in front of them ready to prepare."
CAN YOU AVOID IT?
You cannot tell simply by looking at, smelling or tasting your meal whether it will give you food poisoning. You would never eat food that smells or looks ''off'', but the bugs that cause food poisoning don't change the appearance of food.
It can occur at the biggest and the best establishments. Last month, leading British chef Heston Blumenthal temporarily closed his London restaurant Dinner after several customers fell ill. Westminster health authorities confirmed the cause as norovirus, the same vomit-inducing virus that forced another Blumenthal restaurant to close in 2009. Back then the cause was oysters contaminated with raw sewage. Last month local food authorities suggested poor staff hygiene.
In Australia, in an attempt to weed out dodgy food businesses, the NSW Food Authority has been using its website to name and shame businesses fined for breaches of food regulations. "The trouble with this system is that someone can be named for something as simple as missing hand towels or having a cracked tile," says John Hart, chief executive of Restaurant and Catering Australia. Instead, he suggests looking for five-star safe food stickers on premises' front windows. This is a program initiated by local councils in which businesses are rewarded with higher scores the closer they are to 100 per cent compliance.
"You have to see this is in perspective. Roughly 430 people each month fall ill from food poisoning from eating meals outside the home," says Hart. "That is from 100 million meals prepared in the same time. That's two people per million meals. It's not perfect, but we're one of the safest countries in the world.''
THE FALLOUT
Brett Graham is the co-owner of the Bottle of Milk in Torquay. At the time of writing his cafe was still closed, three weeks after the food poisoning outbreak was identified. He has scrubbed his business from floor to ceiling, spent $20,000 rebuilding the kitchen, complete with new fridges and dishwashers, and installed a window so diners can look in. "No one intentionally tries to make someone sick. I, we [he has a business partner], we feel terrible," he says. "It's a small town and a lot of people we know personally have been affected."
The business is still paying their staff of 20.
"We are voluntarily doing everything we can to regain the trust of our customers," says Graham's business partner, Nick Cogger.
What happens to their business now is in the hands of the authorities and, perhaps, the legal system.
Seventy-seven diners who fell ill after eating at Canberra restaurant Copa Brazilian Churrasco last year are at present taking civil action against its owners in the ACT Supreme Court. A total of 140 people fell ill, with 15 taken to hospital, after eating home-made mayonnaise at the restaurant in May last year.
THE RECOVERY
Ash Lewis is back up and running around. His body is doing as it was before he became ill. There is still the concern, albeit small, that Ash may suffer from medium-term reactive arthritis, a side effect of salmonella poisoning.
Ash's mum, Sarina, is philosophical about her family's ordeal. "I would not rush back to eat there [the Bottle of Milk] but I hold no grudges," says Lewis.
Sarina Lewis is a contributing writer to Good Food.
Food safety at home
● Advice from the Food Safety Information Council is to wash hands before handling food and after using the toilet, coughing or sneezing, changing nappies, handling pets or touching soil.
● To avoid cross-contamination, wash chopping boards and knives before and after use.
● Use separate chopping boards for raw poultry, raw red meat, cooked meats and fresh fruit and vegetables.
● When shopping, pack raw meat and especially poultry separately from each other and from other food.
● Keep food out of the danger zone - temperatures between 5 degrees and 65 degrees where bacteria can thrive. Problems arise with at-risk foods such as raw egg mayonnaise when temperature control is ignored. The solution is to make a small quantity and keep it refrigerated, or if making a larger quantity, divide into small containers, allowing only a small amount to be out of refrigeration at a time.
● At-risk foods include: meat, poultry, dairy products, eggs, smallgoods, charcuterie, seafood, cooked rice, cooked pasta, prepared salads and prepared fruit salads.
Source: Victorian Department of Health and Food Safety Information Council
